Diagnosing Facial Nerve Paralysis: What to Expect at Your Consultation
- Gautham Ullas
- Nov 10, 2025
- 6 min read
Walking into your first consultation for facial nerve paralysis can feel overwhelming. You probably have questions racing through your mind: what will the doctor ask? How long will this take? What tests will I need? Don't worry, I'm here to walk you through exactly what happens during your consultation so you know what to expect.
Your Medical History Comes First
Before any physical examination begins, your surgeon will want to understand your story. This conversation is crucial because facial nerve paralysis can have many different causes, and the details you provide help narrow down what might be happening.
You'll be asked when you first noticed the weakness. Did it happen suddenly overnight, or did it develop gradually over days or weeks? This timing matters more than you might think: sudden onset often points to different causes than gradual weakness.
Your doctor will also want to know about any symptoms that came before the paralysis. Did you have any pain behind your ear? A rash around your face or ear? Any recent cold or flu symptoms? These seemingly unrelated details can provide important clues.
Be ready to discuss any recent travel, especially to areas where Lyme disease is common. Tick bites, even ones you might not remember, can sometimes lead to facial paralysis. Your surgeon will also ask about any recent vaccinations, new medications, or significant stress in your life.
Don't be surprised if you're asked about other symptoms you might not have connected to your facial paralysis. Things like changes in taste, hearing problems, dry eyes, or difficulty eating all help paint a complete picture of what's happening with your facial nerve.

The Physical Examination Process
Once your surgeon has heard your story, it's time for the hands-on evaluation. This part might feel a bit awkward at first, but remember: your surgeon does this regularly and wants to help you feel comfortable throughout the process.
You'll be asked to perform various facial movements while your surgeon watches carefully. This might include:
Raising your eyebrows
Closing your eyes tightly
Smiling with your teeth showing
Pursing your lips like you're whistling
Puffing out your cheeks
Wrinkling your nose
Your surgeon is looking at how well each side of your face moves and comparing them. They're also checking for any unusual movements: sometimes when one part of your face tries to move, another part moves too. This is called synkinesis, and it's important to identify.
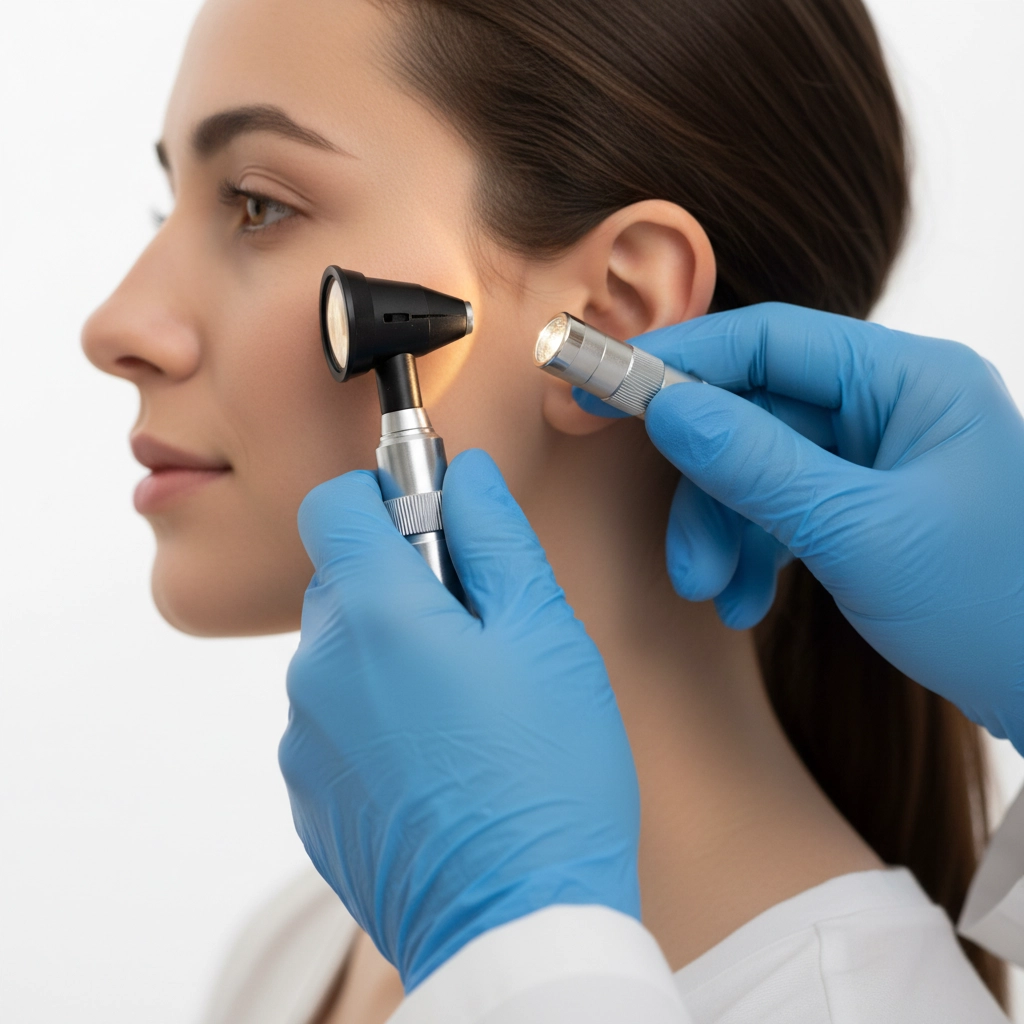
The examination extends beyond just facial movements. Your surgeon will look inside your ears with an otoscope, checking for signs of infection or other problems. They'll also examine your mouth and throat, and gently feel around your neck and the area near your ears.
One test that might seem strange is when your surgeon checks your blink reflex. They'll lightly touch the corner of your eye with a tissue or cotton swab to see if both eyes blink normally. This tests a different part of the facial nerve pathway.
Specialized Tests You Might Encounter
Depending on your specific situation, your surgeon might perform additional tests right there in the office. Don't worry: none of these are painful, though some might feel a bit odd.
A Schirmer test measures how well your eyes produce tears. Your surgeon will place a small strip of special paper in your lower eyelid and wait a few minutes to see how much the paper gets wet. This helps determine if the facial nerve damage is affecting your tear production.
You might also have taste testing on different parts of your tongue. The facial nerve carries taste sensation from certain areas, so changes in taste can help pinpoint where the problem might be along the nerve.
Some patients need hearing tests, especially if they've noticed any hearing changes. The facial nerve runs very close to the hearing nerve, so problems in that area can sometimes affect both.
Imaging Studies: Getting a Closer Look
Not everyone needs imaging studies, but if your surgeon recommends them, here's what to expect. The most common imaging test is an MRI scan, which gives detailed pictures of your facial nerve and the surrounding structures.
If you need an MRI, you'll lie on a table that slides into a large tube. The machine is loud, but you'll be given earplugs or headphones. The scan usually takes about 30-45 minutes. Sometimes you'll receive a contrast injection through an IV: this helps highlight areas of inflammation or other problems.
CT scans are less common but might be needed if your surgeon suspects certain specific causes. These are quicker than MRIs and don't require you to lie still for as long.
The good news is that most imaging can wait a few days or even weeks if needed. Your surgeon will prioritize urgent treatments (like protecting your eye) before getting imaging studies.
Electrical Testing of Your Nerves
In some cases, especially if your paralysis is recent, your surgeon might recommend electrical tests of your facial nerve. These tests have complicated names: electromyography (EMG) and electroneurography (ENOG): but they're basically ways to measure how well your nerve is working.
These tests involve placing small electrodes on your face and sometimes inserting very thin needles into facial muscles. You might feel some mild discomfort, similar to getting an injection, but most patients tolerate these tests well.
The electrical tests work best within the first few weeks after facial paralysis begins, so don't worry if your surgeon doesn't recommend them if you've had symptoms for a long time.

Blood Tests and Other Laboratory Work
Sometimes your surgeon will order blood tests to look for specific causes of facial paralysis. This might include tests for Lyme disease, diabetes, or other conditions that can affect nerves.
Most blood tests can be done right in the office or at a nearby lab. You'll get results within a few days, and your surgeon will call you if anything needs immediate attention.
Grading Your Paralysis
During your examination, your surgeon will assign a grade to your facial paralysis usingone of several tools.
Don't be discouraged by the number: this is just a tool to help measure improvement. Even patients with higher grades can often see significant improvement with proper treatment.
What Happens After Your Consultation
At the end of your visit, your surgeon will discuss their initial thoughts about what might be causing your facial paralysis. Sometimes they can give you a clear diagnosis right away, but other times they might need to wait for test results.
You'll receive a clear plan for next steps. This might include:
Starting medications to reduce inflammation
Beginning eye protection measures
Scheduling follow-up appointments
Arranging additional tests
Referring you to other specialists if needed
Your surgeon will also discuss timeline expectations. Some types of facial paralysis improve quickly, while others take months or even require surgical intervention.
Questions to Ask During Your Visit
Don't hesitate to ask questions during your consultation. Here are some good ones to consider:
What do you think is causing my facial paralysis?
How likely is it to improve on its own?
What can I do at home to help?
When should I be concerned about my symptoms getting worse?
How often should I follow up with you?
Preparing for Your Consultation
To make the most of your visit, bring a list of all medications you're taking, including supplements. If you have any old photos showing your face before the paralysis began, these can be helpful for comparison.
Write down your questions beforehand: it's easy to forget them when you're in the appointment. If possible, bring a family member or friend who can help remember important information.
Remember, getting a thorough evaluation for facial nerve paralysis takes time, and that's a good thing. Your surgeon wants to understand exactly what's happening so they can provide you with the best possible care. The consultation process might feel long, but each step brings you closer to the right diagnosis and treatment plan.
The most important thing to remember is that you're not alone in this journey. Your surgical team has helped many patients with facial nerve paralysis, and they're committed to helping you achieve the best possible outcome.
Ready to take the next step? You can book your consultation to begin your evaluation and get the answers you need.





Comments